Aileen Marshall
Not many of us around the Tri-Institutional community have experienced a pandemic situation like COVID-19. News pundits and politicians are saying this is “unprecedented.” But is it? The word “pandemic” reminded me of references to the so-called Spanish Flu of 1918. Though that event was caused by an influenza virus, from a different family than the current SARS-CoV-2 coronavirus, there are similarities between that outbreak and the current one. Perhaps we can learn lessons from the pandemic that happened almost 100 years ago.
The influenza pandemic started in the spring of 1918 and lasted until the spring of 1919 during World War I. The Allied countries didn’t want people to panic or to distract from the war effort, so they censored reports of the new virulent flu. Spain was neutral, so most reports of the flu came from their newspapers; thus, it became known as the Spanish flu. However, the actual origin of the flu is still unclear.
There are three current hypotheses as to where the 1918 influenza virus started: Kansas, France, or China. A flu-like illness started appearing in Camp Funston in Fort Riley, Kansas in late 1917. It was first reported on March 11th, 1918. At that point more than 100 soldiers had gotten sick and it was spreading quickly. Troops from this camp were shipped to Europe shortly after. Some say that this was not the origin because there was a deadlier flu in New York City at the same time. A 2018 review of the origins of the 1918 pandemic suggests that viral haemagglutinin proteins found in the samples from Kansas were older than those of the 1918 flu. Some think the virus first showed up in Étaples, France in late 1917 where there was an English military camp that was overcrowded with hundreds of thousands of soldiers passing through every day. Pigs and poultry were also kept at the camp, animals suspected of being carriers of the flu strain. And some think this flu started in China, although it’s hard to tell given that records from the country at the time are very sparse. There was a mild flu there at the time, and tens of thousands of Chinese workers toiled behind the French and English lines of the war. A 2018 study by evolutionary biologist Michael Worobey showed that there was no evidence of this flu along the routes the Chinese migrants traveled to Europe, suggesting that China might not have been the origin. This first wave lasted through the spring of 1918.
The second wave started in August of that year and was deadlier than the first. New flu cases started appearing in France, Sierra Leone, and the United States. This time, predominantly young adults were affected. At Army and Navy training camps outside of Boston, almost half of the soldiers died. Worsening the spread, sick soldiers were often sent on crowded trains to crowded hospitals. In September of 1918, New York City started mandating that flu diagnoses be reported and requiring sick patients to be isolated at home. Many cities closed theaters, schools, churches, and bars and banned public gatherings. Philadelphia, however, decided to go ahead with a war bonds parade. Within days of the parade, tens of thousands were sick, and within ten days, over 1,000 people died. October of 1918 was the deadliest month of the pandemic. The United States recorded 195,000 deaths from the flu. Regulations banning spitting in public were passed. In November, news articles about the disease started appearing more frequently as the virus moved from France to Spain. Quarantine signs were put on the homes of people diagnosed with the flu. Yet this same month, people gathered in large numbers to celebrate Armistice Day. As the second wave ended in December, public health campaigns appeared instructing people to put their tissues in the garbage after sneezing into them. Officials asked businesses to stagger their opening and closing times and for people to walk to work to limit crowding on mass transit. The death rate overwhelmed morgues and bodies piled up.
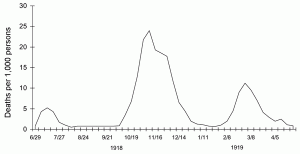
A third, but smaller wave began in February of 1919. In New York City, only about 700 diagnoses and sixty-seven flu deaths were recorded. During this wave, city hospitals around the country set up studies of treatments for influenza. Efforts were made to implement more nursing school programs to address the nursing shortage created by the pandemic. It is now recognized that this shortage was partially due to a societal reluctance to hire African-American nurses. Near the end of the pandemic, President Woodrow Wilson collapsed during the Versailles Peace Conference in April of 1919; it is thought that he also contracted the flu.
Thanks to studies over the last few decades, we now know that the 1918 influenza virus was an H1N1 strain, the same type that caused the swine flu epidemic in 2009. Our knowledge of the strain comes from preserved bodies in the permafrost in Alaska, where the pandemic had been particularly lethal to Native Americans, wiping out entire Inuit villages. In 2008, scientists were able to exhume one of the bodies and obtain tissue samples containing the virus. Because of the extreme cold, the viral particles were relatively well-preserved, and they were able to sequence its genome. A study by the Armed Forces Institute of Pathology, the United States Department of Agriculture, and Mount Sinai Medical School determined that a set of three genes enabled the virus to weaken bronchial tubes, which allowed for secondary bacterial infection, such as pneumonia.
It is now thought that the 1918 flu virus spread so easily throughout the world due to several factors, including military troop movements. Many military installations were overcrowded, and more soldiers died from the flu than in battle. Malnutrition and poor hygiene were more common than today. Interestingly, the flu particularly struck people under age 65, which accounted for almost 90% of the fatalities. This was because influenza caused what is called a “cytokine storm,” an overreaction of the immune system, so young adults with stronger immune systems had stronger overreactions. Furthermore, the disease was not well-diagnosed, as it often caused bleeding in mucus membranes, a symptom not usually characteristic of the flu. There were no antiviral drugs available at the time. It is estimated that about 500 million individuals around the world were infected during the course of the pandemic, or about 25% of the world population. In the U.S., about 28% of the population, almost twenty-nine million, became infected.
Global fatality estimates run from seventeen million to 100 million, or from 1% to 5% of the world. Estimated deaths for the U.S. run from 500,000 to 675,000, or around 0.5 % of the country’s population. Doctors would prescribe 8-30 grams of aspirin, which we now know is toxic. In fact, many deaths were due to aspirin poisoning. There was a high fatality rate among pregnant women. Studies have shown that children born to infected women had lower education levels and socioeconomic status than the general population.
Research has shown that cities like Saint Louis, which had early and sustained practices of social distancing and quarantining the sick, were effective in reducing the spread and had very low fatalities. Saint Louis is often compared to the aforementioned situation in Philadelphia that had little intervention and high numbers of deaths. While these effective practices are similar to the situation with COVID-19 today, a significant difference is that influenza was infectious only during onset of symptoms, not like the asymptomatic transmission that is thought to be possible with this current coronavirus. While there are many parallels between the 1918 flu and COVID-19 pandemics, as of this writing, the global number of deaths from SARS-CoV-2 is 128,000 with 26,000 in the U.S., representing about 0.002% of the current population, five hundred times lower than during the flu pandemic a hundred years ago. Nutrition, hygiene, medicine, and communication have significantly improved during the last century. Remember to wash your hands several times a day, avoid touching your face, and distance yourself from crowds so that hopefully this current pandemic will become part of the history books soon.

(image courtesy of National Archives)
