Part II: Karl Landsteiner, 1930 Prize in Physiology or Medicine
By Joseph Luna
 “Blood is a quite peculiar juice.” When the German poet, statesman and erstwhile scientist Goethe wrote those words in the early 1800s, he might as well have been paraphrasing a problem that physicians had been encountering for at least 150 years prior. It was apparent, since antiquity, that blood is essential for life. And as blood largely looked and behaved the same, it wasn’t a great leap to consider transfusing blood from one being to save another. The realities however, were disastrous: foreign blood would clump (agglutinate) inside a recipient patient, leading to rapid destruction of the incoming blood, followed by hemorrhage and death. Animal-to-human transfusions were performed as early as the mid-17th century with occasional success, but the procedure was risky, often fatal and complicated by religious concerns. Human-to-human transfusions were no different and were considered only as a last resort by the 19th century. Absent a scientific explanation as to why blood transfusions sometimes saved or sometimes killed, with no apparent pattern, religious or supernatural explanations naturally attempted to fill the void.
“Blood is a quite peculiar juice.” When the German poet, statesman and erstwhile scientist Goethe wrote those words in the early 1800s, he might as well have been paraphrasing a problem that physicians had been encountering for at least 150 years prior. It was apparent, since antiquity, that blood is essential for life. And as blood largely looked and behaved the same, it wasn’t a great leap to consider transfusing blood from one being to save another. The realities however, were disastrous: foreign blood would clump (agglutinate) inside a recipient patient, leading to rapid destruction of the incoming blood, followed by hemorrhage and death. Animal-to-human transfusions were performed as early as the mid-17th century with occasional success, but the procedure was risky, often fatal and complicated by religious concerns. Human-to-human transfusions were no different and were considered only as a last resort by the 19th century. Absent a scientific explanation as to why blood transfusions sometimes saved or sometimes killed, with no apparent pattern, religious or supernatural explanations naturally attempted to fill the void.
That is until 1901. Working in Vienna, a young immunologist named Karl Landsteiner stumbled into solving the incompatibility of blood problem, while at first looking to answer a different question on agglutinization. When Landsteiner started working, blood agglutinization tests had been recently developed to detect if someone was infected with a microbe by mixing the patients’s blood with the microbe. If there was clumping, the patient likely was infected. For many immunologists at the time, it was thought that clumping was thus a characteristic of diseased blood, and so problems with blood transfusions could be explained as undiagnosed pathologies. Landsteiner’s great insight was to first question the pathology premise by asking if normal blood clumped. And who could be more normal, he figured, than he and his lab mates.
Landsteiner gathered the men and women in the lab and bled them, himself included. He then separated the two components of blood, the serum (the relatively clear liquid part) from the red blood cells. Upon mixing the serum from one person with the blood cells of another, he observed clumping, suggesting that agglutinization wasn’t pathological, it was found in the otherwise normal people in the lab. He then took it a step further by trying every combination of serum plus blood from his lab mates. To everyone’s surprise, it was not random (see image below). The top table shows the results of men in the lab when one’s serum on the y-axis was mixed with the others blood on the x-axis. By the pattern of pluses (clumping) and minuses (no clumping), it became quickly clear that each person fell within one of three types. Dr. Sturli and Dr. Erdheim had the same clumping pattern (called A); Dr. Pletchnig and Landsteiner’s assistant Zaritsch “Zar” had another (called B); and still another was found in Dr. Störk and Landsteiner himself (called C, but later O). Summarized in the lower table, he performed the same test on six women, all mothers, and found the same result: three basic blood groups. The practical implications to match donors with recipients by type were immediately apparent for safe transfusions.
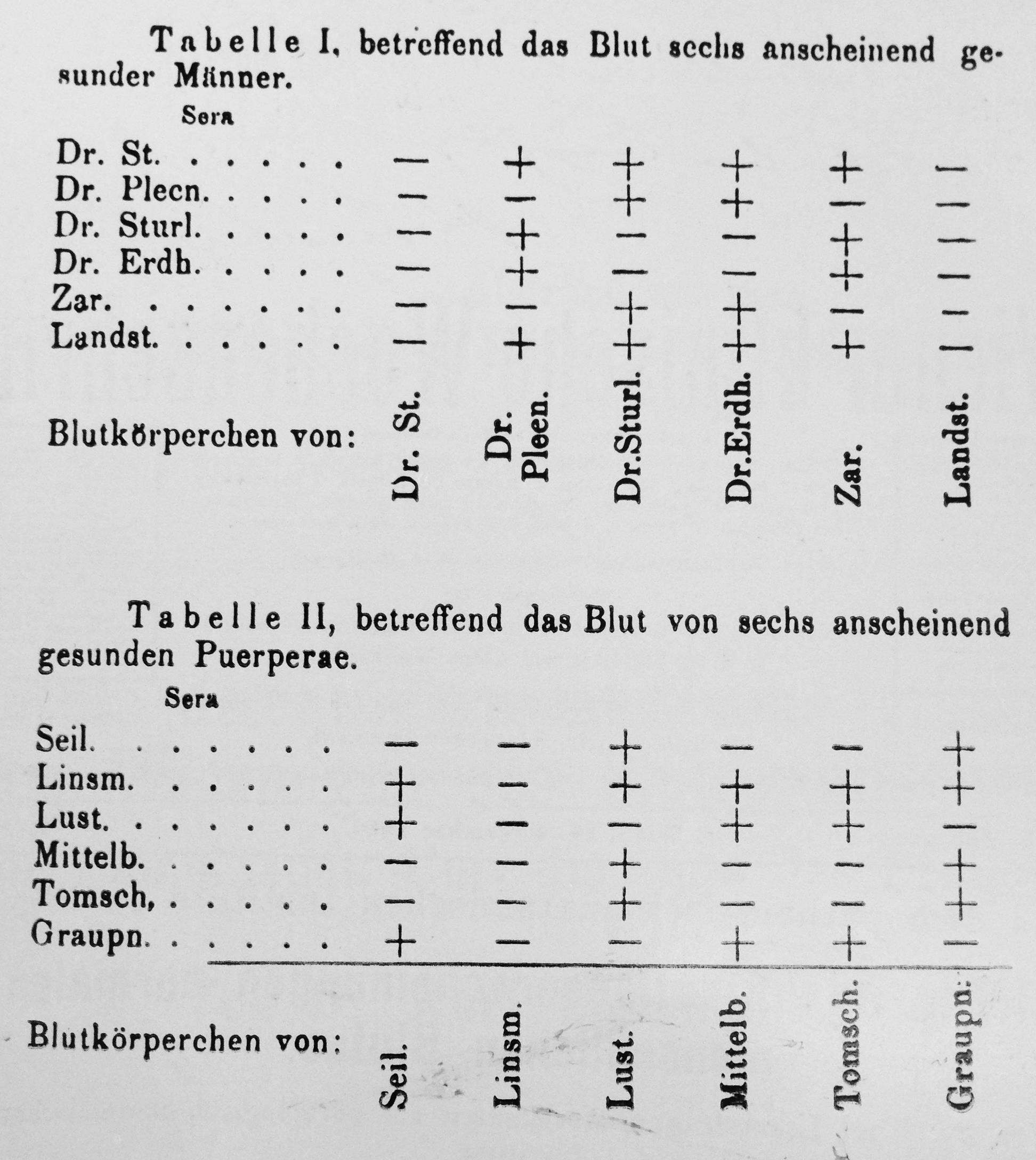 These twelve men and women were the first to be blood typed. By the time of the Great War, this basic test was performed hundreds of thousands of times before blood donation to save soldiers at front lines on both sides. Landsteiner had moved onto other problems by then, all geared toward trying to explain what chemically made an immune reaction so specific, but life in wartime Austria was difficult. He worked a series of jobs at hospitals throughout Vienna during the war and afterwards in Holland, where although he was a world famous immunologist, he performed routine pathology work for a hospital during the day to make ends meet. It was then, in 1922, that he received a lifeline back to the bench: an offer to join The Rockefeller Institute in New York.
These twelve men and women were the first to be blood typed. By the time of the Great War, this basic test was performed hundreds of thousands of times before blood donation to save soldiers at front lines on both sides. Landsteiner had moved onto other problems by then, all geared toward trying to explain what chemically made an immune reaction so specific, but life in wartime Austria was difficult. He worked a series of jobs at hospitals throughout Vienna during the war and afterwards in Holland, where although he was a world famous immunologist, he performed routine pathology work for a hospital during the day to make ends meet. It was then, in 1922, that he received a lifeline back to the bench: an offer to join The Rockefeller Institute in New York.
Karl Landsteiner was in his mid-50s when he arrived in America in 1923. Nowadays he could be considered a mid-career hire, but at the time most viewed his appointment as one of a man already near retirement. Landsteiner proved everyone wrong. He worked and made great contributions to basic immunology, from studies on adjuvants to antibodies to allergies, and trained scores of scientists. And it was at Rockefeller that he returned to studying blood groups and discovered the Rhesus (Rh) factor, whose presence or absence explained the occasional but serious incompatibilities between matched blood types, and is the reason blood types in popular usage are always A-positive or O-negative.
It is estimated that one billion people have been saved through blood transfusions made possible with knowledge of blood groups. It is perhaps fitting then, that Landsteiner was among those with type O. He was a universal donor.
